Research advances in the development of a therapy for yellow fever
04/05/2023
Maíra Menezes (IOC/Fiocruz)
Considered highly safe, the yellow fever vaccine saves thousands of lives annually, especially during outbreaks of the disease. However, vaccination coverage in the population is not always complete and there are certain groups that cannot receive the immunizer due to possible adverse reactions, such as pregnant women, the elderly, people with weakened immune systems, or those who are allergic to egg elements (one of the vaccine compounds). Thus, non-immunization represents a serious risk to life. With no drugs available against the virus, the death rate is between 20% and 60% of cases.
Transmitted by wild mosquitoes, such as Haemagogus janthinomys, yellow fever caused more than 700 deaths in the epidemic recorded between 2016 and 2019 in Brazil (photo: Josué Damacena/Fiocruz)
The development of modern therapy against the disease could change this scenario. In animal tests, a study that had the participation of the Oswaldo Cruz Institute (IOC/Fiocruz) demonstrated the effectiveness of synthetic antibodies against yellow fever. In rhesus monkeys, which develop the disease much like humans, the tested compounds were able to stop the infection from getting worse and prevent deaths. Published in the scientific journal Science Translational Medicine, the research was led by two American institutions: Oregon Health & Science University and George Washington University. The work also had the participation of the University of São Paulo (USP), in addition to other international institutions.
“It is a very important result because it demonstrates that the antibodies are effective in a highly susceptible model”, says researcher Myrna Bonaldo, deputy head of the Laboratory of Experimental Medicine and Health at IOC/Fiocruz. According to the scientist, the next stage of the work should be the manufacturing of a batch of antibodies, following procedures of good manufacturing practices, in order to perform tests on humans. “If its effectiveness is confirmed, it will be a very important treatment for cases of severe yellow fever, in which approximately half of the patients die. It could be a therapeutic tool to save many people”, completes Myrna.
Action against the virus circulating in Brazil
Synthetic antibodies, called monoclonal antibodies, are produced in the laboratory. These molecules reproduce the structure of the antibodies produced by the human body to fight invading microorganisms. In the case of the tested antibodies, the molecules were produced after the scientists had mapped 1,200 antibodies produced by the defense system of people vaccinated against yellow fever.
To arrive at the best compounds, the study began with a screening of 37 molecules. In the United States, they were tested against the vaccine virus, an attenuated version of the African yellow fever virus, used in the manufacturing of vaccines since the 1930s. They were also assessed against a strain isolated from a Senegalese patient in 1965. Capable of causing disease, this strain is routinely used in research.
The five most effective antibodies to neutralize these viruses were sent to the Laboratory of Experimental Medicine and Health at the IOC, on the campus of Fiocruz, in Rio de Janeiro. There, the molecules were tested by Myrna and researcher Lidiane Raphael against three strains isolated from cases recorded in recent outbreaks in Brazil, one in Rio Grande do Sul, in 2008; one in Rio de Janeiro, in 2016; and one in Goiás, in 2017.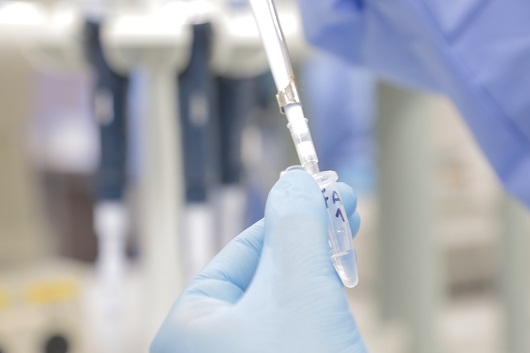
At the Oswaldo Cruz Institute, researchers confirmed that selected monoclonal antibodies are capable of blocking the yellow fever virus circulating in Brazil (photo: Josué Damacena/Fiocruz)
This stage was important because, in a previous study, the scientists had observed that antibodies active against the vaccine virus and African strains may be less effective against the Brazilian viruses, which belong to the South American strain. At the time, the researchers identified mutations in the genome of Brazilian pathogens, which alter the structure of the viral particle, making it difficult for some antibodies to act.
Fortunately, in the assessment of the selected synthetic antibodies, the results were positive. The five molecules managed to block the virus circulating in Brazil. “The vaccine works very well because it induces a repertoire of antibodies. So, even if some of them have a weaker action against Brazilian viruses, others provide protection. However, to develop a therapy, we need antibodies capable of acting in isolation against different viruses. That is what we have identified”, commented Myrna.
Protection against severe disease
Based on the results in the laboratory, two molecules, then, were referred to be tested on animals, performed in the United States. The first tests were performed on hamsters, considered models for studying the disease. With the success of the therapy in rodents, trials were conducted in monkeys, which are affected by yellow fever in a similar way to humans.
The two tested antibodies were effective. All ten treated monkeys survived the infection and none showed liver damage – an organ highly affected by the virus. The presence of the yellow fever virus in the blood of primates has also become undetectable.
During the tests, two monkeys did not receive the treatment and were considered controls. Additionally, the researchers included, in the control group, data from six primates, which had been infected using the same methods in a previous study. Thus, they minimized the use of animals in research, respecting ethical criteria.
Confirming the severity of yellow fever in the absence of treatment, in this group of eight animals, seven developed severe disease. For the authors of the study, the results indicate that the tested monoclonal antibodies can save lives and should be referred for the clinical development of a therapy, with tests in human beings.
Biotechnology advance
Monoclonal antibodies are a type of modern medicine. The first such treatment hit the market in 1986 and was used to reduce the chance of organ transplant rejection. It took time for other molecules to be produced, but from the 2000s onwards, the number of available formulations became ever greater. In 2021, the US drug regulatory agency approved the 100th medicine of its kind.
Most monoclonal antibodies already approved target the treatment of cancer. Some formulations are aimed at infectious diseases. During the COVID-19 pandemic, for example, monoclonal antibodies were developed to fight Sars-CoV-2. Medicines are also used against inflammation in severe cases of the disease.
Although they have great potential, synthetic antibodies pose a challenge: The high cost of production. In this context, the authors of the research point out that, in addition to the risk of death, severe cases of yellow fever can lead to fulminant hepatitis. In 2018, five liver transplants were performed in São Paulo due to the disease.
Scientists say that, considering the costs in the United States, the initial production of the antibodies would cost the equivalent of the value of ten transplants. “It is an expensive product, but the price is feasible for a drug. With the growth of this area in recent years, even more so after COVID-19, producing a monoclonal antibody is much more feasible today than it was ten years ago”, says Myrna.
Importance of vaccination
In the last epidemic recorded in Brazil, between 2016 and 2019, about 2,200 cases were recorded and 759 people died. Myrna points out that low vaccination coverage fueled the epidemic, contributing to the large number of deaths.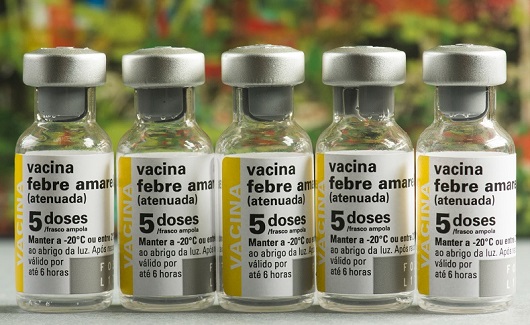
Manufactured by Bio-Manguinhos/Fiocruz, the yellow fever vaccine is offered free of charge by the Brazilian Unified Health System (photo: Rodrigo Méxas/Fiocruz Imagens)
“The vaccine is there. It is extremely effective and will continue to be the main measure against yellow fever, even with the development of a therapy”, emphasizes the researcher, adding that the treatment aims to expand the arsenal against the disease. “In addition to the cases of people who, for some reason, were not vaccinated, the disease can break out in a new area, where there was no recommendation to use the vaccine. There are also some individuals who develop an immune response that lasts for a shorter period after vaccination. In these cases, the availability of immunotherapy is very interesting”, lists Myrna.
The yellow fever vaccine is offered free of charge by the Brazilian Unified Health System (SUS) and recommended by the Ministry of Health throughout the country. Children should receive the first dose at nine months and a booster at 4 years old. Every adult who has not yet received the vaccine or was vaccinated before the age of five should be vaccinated.
The immunizer is only contraindicated for people with severe egg allergy and reduced immunity, such as people living with HIV and a CD4 cell count of less than 350, who are undergoing chemotherapy or radiotherapy, who have autoimmune diseases or who are undergoing treatment with immunosuppressants.




