Fiocruz research shows social impacts of Zika virus
11/12/2018
Fiocruz Bahia
In Brazil, a mother is as vulnerable as her child born with microcephaly due to zika in the last three years, as well as the other women involved in this child daily care. With a systematic routine of doctor’s appointments, stimulation and recovery activities for the child, they had to stop working - which impacts family income - abandon personal projects and face the difficulties of a health system unprepared to care for their children. This data is part of the research Impactos Sociais e Econômicos da Infecção pelo Vírus Zika (Social and Economic Impacts of Zika Virus Infection) results presented last on Novembro 30th at Fiocruz Pernambuco. Developed in collaboration by Fiocruz Pernambuco, Fernandes Figueira Institute (IFF/Fiocruz), the Federal University of Pernambuco (UFPE) and the London School of Hygiene and Tropical Medicine, the study shows that grandmothers, aunts and teenage sisters are also important in the therapeutic care routine and house chores.
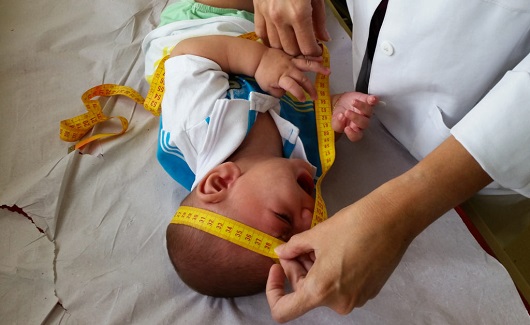
Fathers, when present in the daily lives of these children, are responsible for providing for the family and help in house chores to make mother-centered care lighter. With data collected from May 2017 to January 2018 in the cities of Recife, Jaboatão dos Guararapes (PE), and Rio de Janeiro, the research not only describes the impact of Congenital Zika Syndrome (CZS) in families but also estimated the cost of heath care for children with CZS for the Unified Health System (SUS) and their families - 50% had an income ranging from one to three minimum wages - and identified the impacts in health actions and services, and reproductive health.
The research also showed the average cost with appointments was 657% higher in one year for children with microcephaly or severe developmental delays caused by the syndrome (group 1) compared to children with no impairment (group 3 - control). The number of doctor’s and other health professionals’ appointments increased by 422% and 1,212%, respectively. Family expenses with drugs, hospitalizations and glasses, among others, were 30% and 230% higher compared to children without microcephaly but with CZS manifestations and developmental delay (group 2) and group 3, respectively.
Routine difficulties included insufficient and fragmented health care, with problems in care, lack of communication between specialized services, as well as other complexity levels. For health professionals, the epidemic gave visibility to the difficulties in access that other children with similar problems have determined by other pathologies/congenital syndromes. It also showed that government actions remain focused on the transmitting mosquito and individual prevention, without action on social determinants.
During interviews, most women of reproductive age expressed feeling panic in pregnancy during the zika epidemic. They feared mainly the impact on the child, although they did not fully understand the term Congenital Zika Syndrome. Therefore, they usually referred to it as microcephaly. Uncertainties about how they or their babies could be infected were common. As well as concerns and expressions of suffering regarding the disability and its impact on their lives.
Something else they feared was unplanned pregnancy as they were dissatisfied with the availability of contraceptive methods in health services. Most of them used injectable hormonal contraceptives at the time interviews were conducted and reported lack of information and flaws in the methods used. The IUD did not appear as an option and men were not part of reproductive planning. Almost all the interviewees were unaware of the possibility of having the zika virus transmitted sexually and some heard information about it on television, but they did not give importance because it wasn’t a recurring subject in the media.
There were also uncertainties regarding the possibilities of transmission and only a few received information from health professionals. “Given the lack of information and access to contraceptive methods, we ask how are women going to exercise their reproductive autonomy, choose whether or when to become pregnant,” declares Fiocruz Pernambuco researcher Camila Pimentel, who participated in the study. “Epidemiologists already warned to the possibility of a new zika epidemic. Still, other zika-related issues remain open, such as reproductive rights, psychological support and income generation for the mothers of these babies,” ponders Camila.
Mothers and other caregivers of children with CZS, pregnant women, men and women of childbearing age and health professionals were interviewed for the research, totaling 487 people.




