COVID-19: Fiocruz begins clinical trial with anti-hepatitis C drugs
29/04/2021
Cristina Azevedo (Fiocruz News Agency)
Two drugs used against hepatitis C have been proven effective in inhibiting Sars-CoV-2 replication in cells in laboratory studies. The trial is now entering its phase 2: tests in patients. The results of the first phase of the trial, led by researchers of the Oswaldo Cruz Foundation (Fiocruz), were published on April 21 in a paper for the Journal of Antimicrobial Chemotherapy, by Oxford Academic. The results of phase 2 will likely be known in the second semester of 2021.
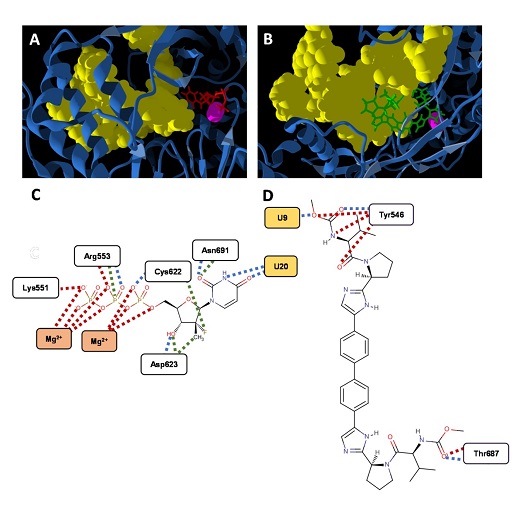
Images show the action of sofosbuvir and daclastavir in a cell infected with Sars-CoV-2
The trial, which began last week, was founded on similarities between the new coronavirus and the hepatitis C virus. If these two drugs were effective against one, they might have results against the other, explains Thiago Moreno, researcher of the Center for Technological Development in Health (CDTS/Fiocruz) and coordinator of the trial which led to the article In vitro antiviral activity of the anti-HCV drugs daclatasvir and sofosbuvir against Sars-CoV-2, the aetiological agent of COVID-19.
The survey showed that daclatasvir was at least seven times more powerful than sofosbuvir and also improved the latter’s potency. Sofosbuvir inhibits viral RNA synthesis by acting directly on the enzyme that helps viruses multiply. Daclatasvir not only inhibited viral RNA synthesis, but also hampered the process through which the virus multiplies its genetic material within the cell. “It made it easier for certain viral RNA structures, which need to be well modeled, to disperse. This means the enzyme that multiplies viral genetic material was not able to function properly”, says Moreno.
During phase 2, which is ongoing with the collaboration of the HCor group and the COVID Coalition (an alliance for research), patients are being given the same dose administered against hepatitis C. But researchers already know that a higher dose might be necessary. With the current dose, the rate of replication inhibition remained between 50% and 95%, considering the peak of the drug and its lower concentration, when the time comes to take the next dose. Ideally, inhibition rate should reach 99.9%.
“Will it be enough to fight Covid-19? I don’t know, but this clinical trial will show us”, says Moreno. If the usual dose fails to work, other dosages will be proposed, but this may force the research to take a step back and return to phase 1 to ensure safety and tolerability even in higher doses.
Using a known drug, the so-called drug repositioning, has advantages and disadvantages as an attempt is made to adapt an old drug to a new disease. “It’s like the wheel of your car got loose because a bolt is missing. You find another one, which is not exactly the same, and try to use it to keep the wheel in place, but you’re not absolutely sure it will work”, says Moreno.
Practicality and price
On the other hand, two of the advantages are price and practicality. Researchers sought drugs available as tablets, to make their administration easier and to make it possible to be used in outpatients. In addition, the company that produces daclatasvir gave up on its patent years ago — this means a generic drug can be produced. The treatment with the drug produced in India costs about US$ 5, says Moreno. At the moment, daclastavir is being used in hospitalized patients with high viral loads, for a better following of the results.
As a comparison, remdesivir, approved by the National Agency of Health Surveillance (Anvisa, the Brazilian equivalent of the FDA) against COVID-19, is applied intravenously, without hospital use; it also uses a more costly technology and is the property of a pharmaceutical company, which also helps make it more expensive.
Although the final paper was only published now, the study was discussed with Anvisa throughout the second half of 2020, and early this year it got the authorization to begin the clinical trial with HCor and the COVID Coalition. “By this year’s second half, we’re likely to have the results of phase 2 and even phase 3”, he says, referring to the increase in scale of the test, with more patients.
The pre-publishing of the study in 2020 drew plenty of international attention. In addition to the groups of CDTS/Fiocruz, the Oswaldo Cruz Institute (IOC/Fiocruz), the Institute of Drug Technology (Farmanguinhos/Fiocruz), the D’Or Institute of Teaching and Research (Idor), and Federal University of Rio de Janeiro (UFRJ), partnerships were made with the Universities of Columbia (USA) and of Liverpool (United Kingdom), which developed complementary researches: while the British institution worked on a prediction of doses, the American worked on enzymatic tests. “This is a very thorough study, providing several layers of evidence regarding the effect of these drugs”, states Moreno.



